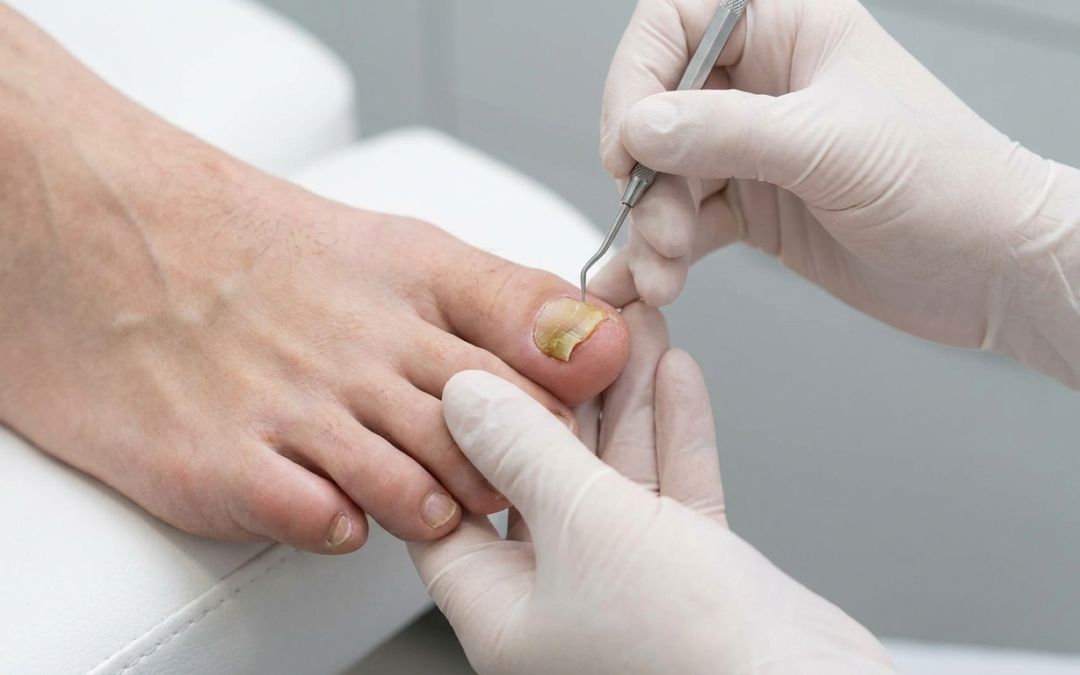
Fungal Toenails in Abbotsford: The Unseen Health Threat Costing You More Than Money
A discoloured, thickened, or brittle toenail is often dismissed as a simple cosmetic annoyance—something to be hidden away in closed-toe shoes. However, what many residents across Abbotsford and surrounding communities like Surrey, Chilliwack, and Langley don’t realize is that toenail fungus, or onychomycosis, is far more than a superficial issue. It’s a progressive infection that carries unseen costs to your health, mobility, and overall quality of life. Industry data reveals a startling truth: ignoring this common condition can lead to significant complications, financial strain from ineffective treatments, and a surprising toll on mental well-being.
Podiatry professionals across British Columbia are increasingly concerned about the number of individuals who delay seeking proper medical care. A study published in February 2024 highlighted that toenail onychomycosis affects an estimated 6.7% of Canadians, with prevalence increasing with age and in those with underlying conditions like diabetes. The real cost isn’t just the price of over-the-counter remedies that often fail; it’s the risk of the infection spreading, causing pain, and potentially leading to more severe health crises.
What Industry Professionals Know About “Harmless” Toenail Fungus
From a podiatrist’s perspective, the term “harmless” is a dangerous misnomer when it comes to onychomycosis. This is not a passive stain on your nail; it is a living, progressive infection caused by fungi that thrive in the warm, dark, and often moist environment inside your shoes. Here’s what experts in foot health understand about the true nature of this condition.
The Cascade Effect: How a Single Nail Can Compromise Your Health
Industry case studies consistently demonstrate a predictable, damaging progression when toenail fungus is left untreated. What begins as a small white or yellow spot under the tip of one nail can quickly escalate.
- Infection Spread: The primary risk is contagion. The fungus can easily spread to other toenails, the surrounding skin (causing athlete’s foot, or tinea pedis), and in some cases, even the fingernails. This turns a localized issue into a widespread dermatological problem that is more complex and costly to treat.
- Pain and Impaired Mobility: As the fungus proliferates, it causes the nail to thicken and become brittle or crumbly. This structural change is not just unsightly; it can create painful pressure inside shoes, making walking, running, or even standing for long periods uncomfortable. Many individuals find themselves altering their gait to compensate, which can lead to secondary musculoskeletal issues.
- Permanent Nail Damage: Chronic, untreated infections can destroy the nail plate and damage the nail bed itself. This can result in permanent deformity of the nail or even cause it to separate from the toe completely (onycholysis). Once the nail bed is scarred, healthy regrowth may become impossible.
- Risk of Secondary Bacterial Infections: A compromised, cracked, or lifting nail loses its protective function. This creates an entry point for bacteria to invade the underlying skin, leading to a serious condition called cellulitis. Cellulitis is a bacterial infection of the skin and deeper tissues that causes redness, swelling, and pain, and can become life-threatening if it enters the bloodstream.
The Financial Drain of Ineffective Treatments
Many Abbotsford residents first turn to pharmacies, purchasing over-the-counter topical creams, lacquers, and home remedies. While seemingly a cost-effective first step, professional experience shows this is often a waste of money and, more importantly, time. Most topical treatments fail because the nail plate (keratin) is non-porous and designed to be a barrier. These products cannot effectively penetrate the nail to reach the fungus living in the nail bed underneath.
Patients often spend hundreds of dollars over months or even years on these remedies, only to see the infection worsen. This delay allows the fungus to become more entrenched, making professional medical treatments, which are more effective, also more intensive and prolonged. The Canadian Dermatology Association notes that even with prescription topicals, cure rates can be low and treatment can take up to a year.
The Connection to Systemic Health: A Red Flag for Diabetics
For individuals in communities from White Rock to Vernon living with diabetes, peripheral vascular disease, or compromised immune systems, toenail fungus is a significant health threat. Podiatrists and endocrinologists across Canada emphasize this connection. Diabetes often causes peripheral neuropathy (nerve damage) and reduced blood flow to the feet.
A person with diabetes may not feel a small cut or pressure sore caused by a thickened fungal nail. Combined with poor circulation that impairs healing, this minor issue can rapidly evolve into a non-healing ulcer. These ulcers are a leading cause of lower-limb amputations. For this high-risk population, treating toenail fungus is not optional; it is an essential component of preventative diabetic foot care.
The Hidden Costs: Quality of Life and Mental Well-Being
Podiatry experts recognize that the impact of onychomycosis extends far beyond physical symptoms. The emotional and social burden is a significant, though often unspoken, cost of living with this condition. The unsightly appearance of fungal nails frequently leads to feelings of embarrassment and self-consciousness.
Industry surveys and patient reports reveal a pattern of avoidance behaviours. People may stop wearing sandals or open-toed shoes, even in the warm Okanagan summers experienced in Penticton and Kelowna. They might avoid swimming pools, yoga classes, or beach outings with family. A Canadian survey found that 50% of respondents with the condition changed their behaviour to hide their feet. This social withdrawal and negative self-image can diminish overall quality of life and contribute to anxiety.
The Professional’s Guide to Effective Fungal Toenail Treatment in BC
Navigating treatment options can be confusing. A podiatrist provides the most crucial first step: an accurate diagnosis. Not all discoloured or thickened nails are caused by fungus; conditions like psoriasis or nail trauma can appear similar. The Canadian Dermatology Association confirms that a lab test is the only way to be certain. Once onychomycosis is confirmed, a podiatrist at a clinic like Island Foot Clinics in Abbotsford can recommend a treatment plan based on the severity of the infection.
Modern Medical Interventions
- Oral Antifungal Medications: For moderate to severe infections, prescription oral medications like terbinafine or itraconazole are often the most effective approach. These drugs work systemically, reaching the nail bed through the bloodstream to attack the fungus from within. While effective, they require a treatment course of several months and may carry potential side effects, necessitating a discussion of your medical history with a podiatrist.
- Advanced Topical Solutions: Newer prescription topical medications, such as efinaconazole, are formulated with enhanced penetration properties. They can be a viable option for mild to moderate cases, especially for patients who cannot take oral medications.
- Laser and Light-Based Therapies: Laser treatment for fungal toenails has emerged as a popular, non-invasive option. At clinics in locations like Victoria, Nanaimo, and Kelowna, specialized medical lasers are used to emit pulses of energy that pass through the nail to the nail bed. This energy heats and destroys the underlying fungus without damaging the surrounding tissue. Multiple sessions are typically required.
- Photodynamic Therapy (PDT): An innovative approach involves applying a light-sensitizing agent to the nail, which is then activated by a specific wavelength of light to destroy fungal cells. This localized treatment avoids the systemic side effects associated with oral medications.
- Debridement: This is a crucial supplementary procedure where a podiatrist mechanically thins the thickened, fungal portion of the nail. This reduces pain from shoe pressure and allows topical medications to penetrate more effectively.
Local Expert FAQ: Your Fungal Toenail Questions Answered
Why can’t I just have the nail removed?
Industry professionals advise that surgical removal of the nail is typically a last resort for severe, painful cases or those that do not respond to other treatments. Simple removal does not eliminate the underlying fungal infection in the nail bed. Without concurrent antifungal treatment, the new nail will likely grow back infected.
Is laser treatment covered by BC’s Medical Services Plan (MSP) or extended health benefits?
The BC Podiatric Medical Association clarifies that laser therapy for toenail fungus is generally considered a cosmetic procedure and is not covered by MSP. While some extended health plans may offer partial coverage for podiatric services, it’s essential to check directly with your provider, as coverage for specific treatments like laser therapy varies widely.
How can I prevent fungal toenails from coming back?
Recurrence is a common challenge. Professional standards of care emphasize preventative measures. This includes keeping feet clean and dry, wearing moisture-wicking socks, using antifungal sprays or powders in your shoes, and avoiding walking barefoot in public damp areas like gym showers and pool decks. It’s also vital to treat any co-existing athlete’s foot infection, as the fungus can easily spread from the skin back to the nails.
I have diabetes. What is the first thing I should do if I suspect a fungal nail?
Experts in diabetic foot care strongly recommend immediate consultation with a podiatrist or your primary care physician. Do not attempt self-treatment or ignore the issue. A podiatrist, such as those specializing in diabetic foot care in Surrey or Abbotsford, can assess your feet for any signs of complications, provide safe nail care, and recommend a treatment plan that considers your overall health status.
Key Takeaways
- Fungal toenails are a progressive medical infection, not just a cosmetic flaw.
- Ignoring the infection can lead to pain, spreading of the fungus, permanent nail damage, and serious bacterial infections like cellulitis.
- For individuals with diabetes, untreated toenail fungus is a significant risk factor for developing foot ulcers and subsequent amputations.
- Over-the-counter treatments are often ineffective and can waste valuable time and money while the infection worsens.
- Professional diagnosis is key, as other conditions can mimic a fungal infection. Modern treatments available at clinics across BC, including oral medications and advanced laser therapies, offer high success rates.
- The unseen costs include a diminished quality of life, embarrassment, and social avoidance.
Your Next Step to Healthy Feet in Abbotsford
Living with the discomfort and embarrassment of fungal toenails is not something you have to accept. The financial, physical, and emotional costs of inaction are far greater than the investment in professional, effective treatment. By seeking expert care from a podiatrist, you are not just treating a nail; you are protecting your overall health, mobility, and well-being.
If you are in Abbotsford, Surrey, Chilliwack, or any of the surrounding communities, the first step is a professional assessment. A correct diagnosis opens the door to a personalized treatment plan that can eradicate the infection and restore your nails to health, allowing you to step back into your life with confidence.
While we aim for accuracy, please verify details for your specific situation. For personalized advice and to discuss how these insights apply to your specific needs, we’d love to chat with you directly.
Don’t let a “simple” nail problem dictate your health and happiness. Contact Island Foot Clinics today to schedule your consultation and take the definitive step towards clear, healthy nails.